Pelvic floor muscle training— A.K.A. Kegels—is a simple, targeted way to build strength and better control in the muscles that sit like a supportive hammock at the base of your pelvis. These muscles hold up important internal parts, and when you train them right, they can help with pesky issues like bladder control.
The catch?
Not every “insertable product” out there is actually doing the job of real training. This article keeps things straight: we’ll cover the real benefits backed by solid guidance, walk you through exactly how to do the exercises along with pelvic floor exercise tips, and clearly separate the legit training tools from the ones that are basically just sex toys with fancy marketing.
Table of Contents
- What the Pelvic Floor Does
- What Pelvic Floor Strengthening Can Actually Help With
- When Strengthening Is a Good Fit — and When It Isn’t
- How to Find the Right Muscles
- How to Do Pelvic Floor Exercises Correctly
- Common Mistakes That Make Kegels Less Effective
- Do You Need a Device at All?
- When to See a Pelvic Floor Physical Therapist or Doctor
- Bottom Line
- Want More Reads?
What the Pelvic Floor Does
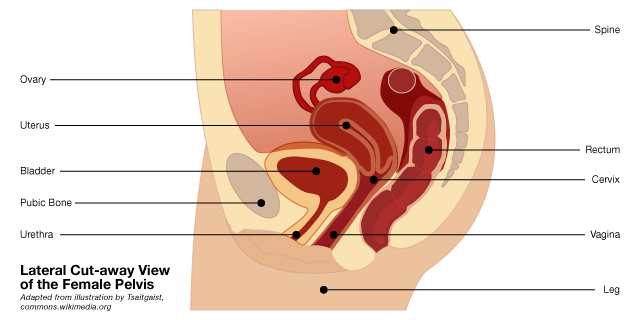
Picture a thin layer of muscles and connective tissue stretched across the bottom of your pelvis, running from your pubic bone in front to your tailbone in back. That’s your pelvic floor. It acts like a dynamic sling that quietly supports your internal organs while also helping manage pressure when you move, laugh, cough, or lift something.
They work together with your deep core and diaphragm to handle changes in pressure inside your belly – think standing up from a chair, carrying groceries, or even just breathing deeply. They also help close off the openings for your urethra and anus at the right times. When everything’s working smoothly, you don’t even notice it. But when coordination or strength dips, that’s when little things start feeling huge. The pelvic floor isn’t just about one job – it’s part of how your whole lower body stays balanced and responsive through daily life.
What Pelvic Floor Strengthening Can Actually Help With
If you leak a little when you cough, sneeze, laugh, run, or jump (classic stress incontinence), pelvic floor muscle training is often the go-to first step. UK guidelines from NICE recommend a supervised program lasting at least three months for women dealing with stress or mixed urinary incontinence, and it can lead to real improvements that sometimes help people skip more invasive options altogether.
It also supports bowel control for some women. The same muscles help manage gas and stool, so strengthening them can ease urgency or accidental leaks there too. For pelvic organ prolapse symptoms (like that heavy or dragging feeling) training can provide extra support and make daily activities more comfortable, especially when started early.
Sexual function gets mentioned a lot online, but the evidence is more measured. Some studies show possible improvements in areas like arousal, orgasm, lubrication, and satisfaction, but a 2024 systematic review rated the certainty of that evidence as low. So it’s fair to say it might help some women feel more confident or comfortable in that department, but it’s not a guaranteed bedroom game-changer for everyone.
The nicest part?
Once you learn the moves, it costs nothing and you can do it anywhere. It’s a practical, low-tech starting point that fits into real life without fancy equipment.
When Strengthening Is a Good Fit — and When It Isn’t

Not every pelvic floor issue boils down to “just do more Kegels.” Some women have muscles that are already too tight or overactive (a hypertonic pelvic floor) and squeezing them more can actually make things worse. Cleveland Clinic notes that this tightness often shows up as ongoing pelvic pain, painful sex, trouble starting or stopping your urine stream, constipation with straining, or a constant clenched feeling in the hips or lower back.
In those cases, the priority is learning to relax and lengthen the muscles first, often with guidance from a pelvic floor physical therapist who can identify what’s really going on. Strengthening shines for women whose muscles are weak or underactive. This is common after pregnancy, childbirth, menopause, or years of high-impact sports. It’s also great as prevention if you’re planning pregnancy or noticing early leaks.
Don’t self-diagnose based on one symptom. If pain, heaviness, or emptying problems are part of the picture, skip the solo exercises and get checked first. A quick professional assessment saves time and prevents frustration.
How to Find the Right Muscles
- Sit or lie down comfortably and imagine you’re trying to stop yourself from passing gas. You should feel a gentle squeeze-and-lift sensation.
- Picture gently lifting a tampon inward and upward, or stopping your urine stream just once as a quick test (never use this as the actual exercise).
- You’ll likely notice a subtle tightening around your vagina and a slight lift toward your belly button.
For extra confirmation if you’re doing it right:
- Wash your hands, insert a clean finger into your vagina, and try the same squeeze. You should feel the walls gently close around your finger without pushing down.
- Practice in different positions like lying down, sitting, and standing to get the feel for it.
Most women need a couple of tries before it clicks, and that’s completely normal. Focus on that inward-and-upward lift, never a bearing-down push.

How to Do Pelvic Floor Exercises Correctly
Once you’ve found the right muscles, follow these simple steps (based on Mayo Clinic guidance):
- Get into a comfortable position – many women start lying on their back with knees bent.
- Take a normal breath in. As you breathe out, gently squeeze and lift your pelvic floor muscles (imagine picking up a marble with your vagina).
- Hold the squeeze for a few seconds.
- Fully relax and let go for the same amount of time.
- Breathe normally throughout – never hold your breath.
- Keep your thighs, buttocks, and stomach relaxed. Only your pelvic floor should be working.
- Focus on slow, controlled movements. The full release is just as important as the squeeze.
Quality matters more than speed. Do the exercises with good form every time.
A Beginner Routine
- Do 8–10 slow holds: squeeze and lift for 3 seconds, relax fully for 3 seconds.
- Follow that with 8–10 quick “flicks” – one-second squeezes and releases.
- Repeat the whole thing three times a day.
- You can mix positions: one set while lying down, one sitting at your desk, one standing.
Over the first couple of weeks, gradually build the hold time to 5–10 seconds as it feels easier. Add in “pre-contraction” habits too – like gently lifting right before you cough, sneeze, or lift something. Many programs suggest mixing slow endurance holds with fast reactions for all-around function. And give it time! Mild improvements might show in 4–6 weeks, but major changes often take the full 3 months that guidelines talk about. Consistency in short daily bursts works better than marathon sessions once a week.
How Long Before You Notice Results?
It depends on your starting point and consistency, but don’t expect overnight miracles. Many women notice easier control or less leakage within 3–6 weeks of daily practice. Stronger contractions and bigger symptom changes usually show up around the 8–12 week mark, with full benefits often taking the 3–4 months that major guidelines recommend.
Factors like technique quality, how often you remember to do the “pre-contraction” habit during daily activities, and whether your issue was mild or more established all play a role. Patience and steady routines pay off way more than pushing hard for quick wins.
Common Mistakes That Make Kegels Less Effective

- Pushing down or bearing down (like you’re trying to have a bowel movement) instead of gently lifting upward. This can actually weaken your support over time.
- Using the wrong muscles by clenching your thighs, buttocks, abs, or inner thighs at the same time. Your pelvic floor needs to work on its own.
- Holding your breath during the squeeze. This turns it into straining instead of controlled training.
- Forgetting to fully relax and release between each repetition.
- Doing random squeezes throughout the day with no plan, progression, or variety.
- Overdoing it or training too intensely without rest days.
- Practicing Kegels while urinating as a regular habit (only use the stop-the-stream feeling once as a test, never as the exercise).
- Expecting dramatic results in just a week or two.
- Ignoring pain or discomfort. It your lower back, stomach, or pelvis hurts afterward, you’re likely doing something wrong.
Do You Need a Device at All?
Plenty of women get great results with nothing but their own body and good technique. If you can feel the squeeze-and-lift and you’re consistent, you’re already ahead of the game. Devices become helpful add-ons when you’re not sure you’re activating the right muscles, you need extra motivation to stick with it, or a therapist recommends them for your specific situation.
They’re not a magic shortcut or a requirement. Think of them like training wheels—useful for some, unnecessary for others. Starting simple keeps things straightforward and helps you build real awareness before adding anything extra.
What Counts as a Real Pelvic Floor Training Device
A true pelvic floor trainer has one clear job: helping you actively strengthen or gain control through a structured program. It should involve resistance, feedback, or a defined therapeutic use – not just being insertable.
The main evidence-backed categories are:
- Vaginal weights or cones: You insert them and actively contract to hold them in place while standing or moving—progressive sets build strength.
- Biofeedback devices: Sensors inside track your contractions and give real-time feedback through an app or screen so you know you’re doing it right.
- Electrical stimulation units: Used as a gentle nudge when someone can’t voluntarily contract well yet; they help “wake up” the muscles as part of a supervised plan.
These tools are tied directly to continence or strengthening goals and often carry medical clearance for that purpose. They support the exercises rather than replacing them.
What Does Not Count as a Pelvic Floor Trainer
A generic vibrating G-spot egg, bullet vibrator, rabbit toy, or any insertable pleasure product marketed with vague “wellness” language doesn’t magically become a trainer just because it goes inside. These are designed for sensation and fun, not for structured muscle resistance or feedback.
They lack the progressive weight system, sensor data, or therapeutic protocol that actual trainers have. Using one might feel nice or help with relaxation in some moments, but it won’t give you the targeted strengthening work that clinical tools provide. The line gets blurry in marketing, so check the actual intended use and features before buying.
How to Judge Whether a Product Is Safe and Legit
Look for clear labeling that states it’s for pelvic floor strengthening or incontinence support, plus step-by-step exercise instructions. Body-safe materials matter most – medical-grade silicone, ABS plastic, borosilicate glass, or stainless steel are nonporous, easy to clean, and don’t harbor bacteria. A 2023 study found that some cheaper toys (especially porous or soft “jelly” types) can release microplastics and nanoplastics during use and contain phthalates above safe levels, so skip anything with vague material descriptions.
Good products include straightforward cleaning directions, realistic claims, and notes on who should avoid them. Reputable brands often list FDA clearance for therapeutic use. If it encourages wearing it all day without guidance or promises miracle results, that’s a red flag.
Are Biofeedback Devices Worth It?
They can be a nice boost for some women who struggle to feel or track their contractions. The 2025 Cochrane review looked at dozens of studies and found that adding biofeedback to regular training gives little to no extra improvement in quality of life and only small, often unimportant differences in leakage episodes compared to exercises alone.
A 2024 JAMA Network Open Randomized Clinical Trial (Wang et al.) did show that a specific pressure-based biofeedback approach helped postpartum women with stress incontinence more than standard training alone. So the answer is personal: worth it if you need the feedback for motivation or accuracy, but not automatically better for everyone. They’re a tool, not a must-have.
When to See a Pelvic Floor Physical Therapist or Doctor
Book an appointment if you have pelvic pain, pain during sex or with tampons, a feeling of heaviness or bulging, trouble fully emptying your bladder or bowels, or no improvement after 8–12 weeks of correct exercises. Postpartum, post-surgery, or menopause changes are also smart times for a check-in.
A pelvic floor PT can assess whether your muscles are tight, weak, or uncoordinated with hands-on evaluation and give you personalized cues. Doctors can rule out other issues and refer you onward. Getting help early often means faster, better results and prevents small problems from growing.
Bottom Line
Pelvic floor strengthening is a legitimate, evidence-based practice that can genuinely improve bladder control, support, and day-to-day comfort when done correctly. Start with the exercises themselves – learn proper technique, stay consistent, and listen to your body. Devices can be helpful extras if you need feedback or resistance, but only the ones built for therapeutic training count as real trainers. Generic vibrating sex toys might feel good, but they’re in a completely different category and shouldn’t be sold or used as strength tools.
The smartest move is simple: focus on good form first, consider professional guidance if anything feels off, and choose any products carefully based on real features rather than marketing. Your pelvic floor is doing important work every single day – give it the right kind of attention, and it will usually repay you with better confidence and fewer leaks. You’ve got this.
If you ARE looking for actual sex toys (for pleasure only) check out Lovense Nora rabbit vibrator, Lush 4 vibrating g-spot egg, and Ferri wearable panty vibrator.
Want More Reads?
- Prostate Massagers for Health – Are They Worth It?
- Is Dead Vaginal Syndrome Real?
- What is Vaginal Atrophy? Estrogen, Sex, and Pain
- How to Clean Your Vagina – Tips to Take Care of Yourself







